HFS updates on the Medicare Medicaid Alignment Initiative (MMAI) transition to Dual Eligible Special Needs Plan (D-SNP)
Date: 01/13/26
On January 9, the Illinois Department of Healthcare and Family Services (HFS) issued a provider notice regarding the transition of the Illinois Medicare-Medicaid Alignment Initiative (MMAI) program to fully integrated dual eligible special needs plans (FIDE SNPs) and the process for verifying FIDE SNP enrollment.
Department Enrollment Systems
UPDATE: Until further notice, if HFS’ enrollment file (e.g. MEDI) lists a FIDE SNP in the Medicare Advantage section and a Health Choice Illinois (HCI) plan in the Managed Care Organization section, the FIDE SNP is the correct plan. See MEDI screen print below as an example. Please note that FIDE SNP enrollment may change monthly because members can switch monthly. Providers should submit claims to the FIDE SNP and not the HCI plan listed.
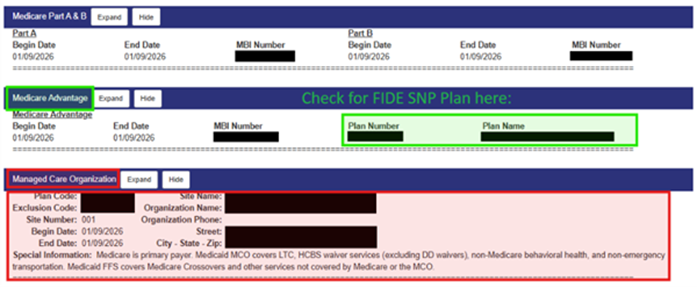
Please note that the special information listed under the Managed Care Organization is incorrect if the member is enrolled in a FIDE SNP.
As stated in the HFS Provider Notice issued 12/24/2025, Meridian’s FIDE SNP will appear as follows in MEDI:
- Wellcare Meridian Dual Align (HMO D-SNP): Contract Number: H6971001, Health Plan Name Displayed in Medi: MERIDIAN HEALTH PLA INC SNP
Per Provider Notice issued 12/24/2025, FIDE SNPs have the most accurate enrollment information because the health plans, not HFS, enroll members in the FIDE SNP program. We encourage all providers to verify enrollment information with Wellcare Meridian Dual Align (HMO D-SNP). To contact Meridian and to verify enrollment, please login to the secure provider portal.
HFS is developing a manual reconciliation process to correct the inaccurate HCI plan enrollment information and when it’s finalized, will issue an updated provider notice. Please email any questions to HFS.DSNPInquiries@Illinois.gov.
